- Monday – Saturday :9:00 AM – 6:00 PM
Our Services
Opening Hours
Contact Info
Main Office
No 35 Pope John Paul II Street,Off Gana Street Maitama,
Abuja Nigeria.
Two of the most significant events in a woman’s life can also lead to a decline in vaginal health:
Childbirth stretches the vaginal canal and surrounding tissue. For many women the body’s own healing response repairs the damage and they return to normal health. For others, however, the tissue will not return to a pre-childbirth state. For these women the damages from stretching the vaginal walls, perineum and surrounding tissues can lead to diminished vaginal health and function.
Menopause results in reduced estrogen levels. Other events such as hysterectomy, chemotherapy, or the process of breast-feeding can also lead to reduced estrogen levels culminating in the thinning, drying and inflammation of the vaginal walls.
What is Laser Vaginal Rejuvenation?
Carbon dioxide laser vaginal rejuvenation is a quick, non-surgical procedure done to restore vaginal health by promoting the remodelling of the vaginal mucous epithelium layer. The regeneration of new tissue within the vaginal walls that takes place following treatment rebuilds a naturally stronger structure, and recovers lost volume, hydration and elasticity.
How does it work?
The basis of the carbon dioxide laser vaginal rejuvenation is fractional photothermolysis. In other words, a probe is inserted into the vagina and optically splits a laser beam into a series of very small dots that are aimed at the inside wall of the vagina. At the point of contact, the laser dot removes a tiny area of tissue. This creates a microscopic pinhole about the size of the diameter of a human hair. As the body repairs itself, it stimulates cells to create new healthy tissue at the site of the dot and immediately surrounding it. The laser also heats the area between the dots, stimulating the activity of specialised cells that create elastin and collagen (the scaffolding components of healthy tissue) which result in vaginal tightening and hydration.
In what situations do we use the Co2 vaginal rejuvenation laser?
In conditions that cause vulvovaginal atrophy (when vaginal lining becomes thinner, dryer and less elastic) due to a drop in the oestrogen levels.
- Menopause
- “Induced” menopause as a result of hysterectomy or suppression of ovarian function by chemotherapy and radiation.
- Breastfeeding related vaginal dryness
- Anti-oestrogen medications such as Goserelin and Leuporolide
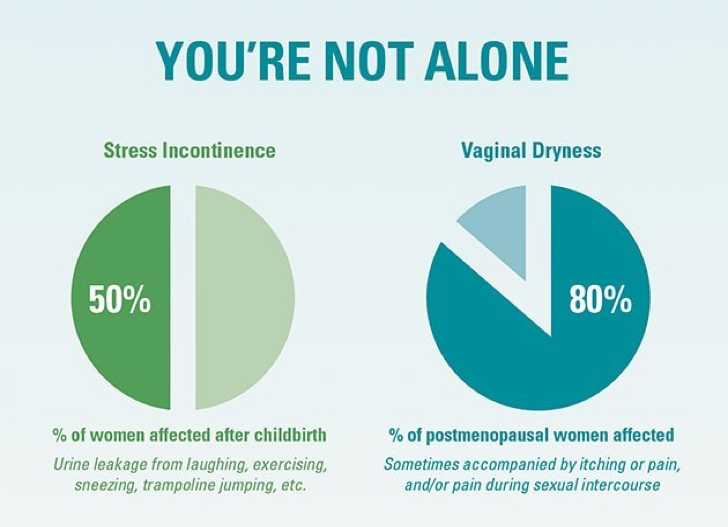
1, Brown JS, Grady D, Ouslander JG, Herzog AR, Varner RE, Posner SF. Prevalence of urinary incontinence and associated risk factors in postmenopausal women. Heart & Estrogen/Progestin Replacement Study (HERS) Research Group. Obstet Gynecol. 1999; 94:66–70.
2, R.E. Nappi, M. Kokot‐Kierepa. Vaginal health: Insights, views & attitudes (VIVA)—Results from an international survey. Climacteric, 15 (2012), pp. 36-44
What to expect during the procedure?
A gynaecological exam will be carried out before the procedure and a topical anaesthetic will be applied on the vulva to further increase comfort, the procedure is generally painless.
Treatment time is 1 hour or less.
What results do I expect after this procedure?
- Improved Stress Urinary Incontinence.
- Improved Vaginal Dryness and Laxity.
- Increased Comfort During Intercourse.
- Naturally Increased Vaginal Lubrication.
Results are noticeable after the first treatment, but 3-5 sessions performed at 4-weekly intervals with a yearly maintenance are recommended for optimum results.
Are there any side effects?
Most women return to their normal activities after the procedure, and can resume sexual intercourse in 72 hours. Side effects are minimal, some patients may experience discomfort, a watery discharge or spotting for up to 48 hours’ post-treatment.
What is the cost of this procedure?
For the cost of this procedure and others, please download our comprehensive pricelist on the “about us” page of this website.
